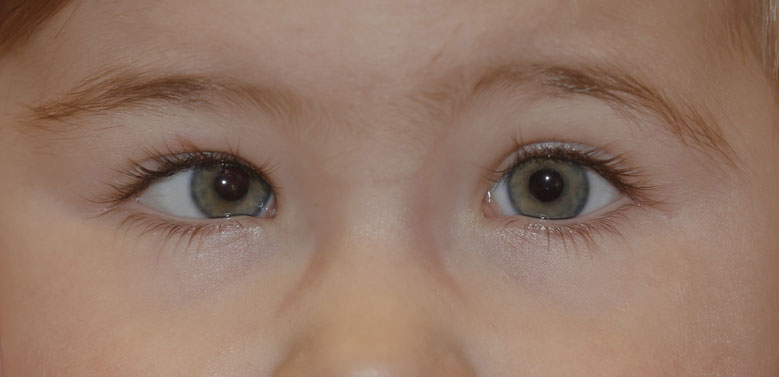
What is congenital strabismus?
Before commenting on what congenital strabismus is, keep in mind that strabismus can be classified in relation to several factors:
- depending on the age of appearance, being able to be congenital or acquired,
- based on the disposition of the deviated eye,
- according to the frequency of appearance,
- by alternating between one eye and the other.
If something characterizes one of them, it is the need for early treatment. We refer to congenital strabismus or also called infant or child. True to our philosophy of preventive medicine, we want to mention the characteristics of this type of deviation and that it is so associated with the youngest patients in our practice.
It is important not to confuse congenital strabismus, whose aforementioned characteristic is the need to be treated early, with other types of strabismus whose early appearance also occurs before 8 months of age. In any case, and under suspicion of strabismus that the parents or the school may have, it will be a reason to carry out an ophthalmological examination regardless of age.
Congenital strabismus is a type of convergent ocular deviation or what we call esotropia. It is observed how the eye is deviated towards the nasal side (nose), that is, inwards. Normally the deviation is of a wide angle not less than 40 prismatic diopters and constant, where the eye will usually have difficulty abducting (moving the eye outwards). In many cases it is accompanied by a vertical type deviation, torticollis and/or nystagmus.
Diagnostic tests
Given the child’s age and lack of ability to cooperate, the Hirschberg test and eye tracking study carried out with an ophthalmoscope torch are very useful when making a diagnosis. An electrophysiological study (for evoked visual potentials) is also recommended to identify asymmetrical vision. In each case, organic conditions will need to be ruled out through a dilated fundus examination.
Causes
Although the origin and cause of strabismus is still a matter for debate, experts agree that it can appear during the first 4 months after birth, although it is more evident from 6 months onwards. Patients that have developmental alterations or that were born prematurely may show this type of ocular deviation, and a family history of strabismus could also be a factor.
Treatment of congenital strabismus
The refraction in the child’s eye must be studied, using cycloplegic or atropine drops, before beginning treatment with optical correction, if necessary. Early surgical intervention is normally advised to correct the deviation. The objectives are both aesthetic and functional, trying to improve binocular vision and help the patient’s vision develop as soon as possible. The treatment will help the child in the future stages of learning that await him or her.
